We believe in providing more than just healthcare..
Elevate Your Wellness Journey
Comprehensive Care, Extraordinary Results
Ensuring you feel valued
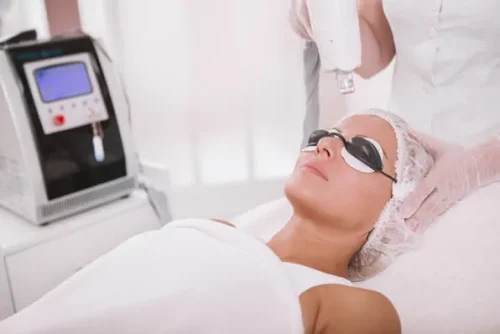
Laser Treatments

Cosmetic Surgery

Injectables

Skin Tightening
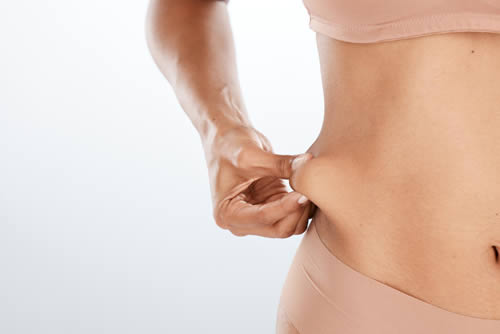
Liposuction
Welcome to Women's Healthcare & Beyond!
At Women’s Healthcare & Beyond, we provide comprehensive gynecologic care and advanced medical aesthetics services. Our mission is to deliver excellent care and treat our patients like family. We offer a modern and professional environment where your health and wellness are our top priorities.
Empowering Women's Health: Our Services
Educational Materials and Blogs
Patients Portal
Testimonials
-
Dr. Bazzi is a wonderful doctor. Very down to earth and caring. Very easy to talk to and she knows her stuff! Would recommend to anyone!!
Sara L -
Dr. Bazzi is the most wonderful doctor I have ever came in contact with! She is such a blessing. She really takes the time with her patients.
Andrea S -
Exceptional! If you’re looking for somewhere to be comfortable then this is the perfect doctor for you!!! 5 out of 5!!!
Shawntae J -
She is an amazing doctor! Would recommend her to anybody. I've been to many other doctors and she is by far the best. She knows exactly what she's talking about.
Amy J -
Dr. Bazzi, well let's just say she's absolutely AMAZING!! I love how honest she always is, makes you feel very comfortable, and educates you very well!
Sarah D -
There's no way possible I would be able to say anything bad about Dr. Bazzi. She is so down to earth. I felt comfortable with her the first time I met her. No matter what you're seeing her for, she is straight forward, compassionate, she explains everything in a way that you can understand. I highly highly recommend her for all your feminine needs.
Melanie G -
Dr. Bazzi is amazing! She pushed for all the right tests to be done and even came to check up on me while I was admitted. I've never come across a doctor who cared so much about their patients and helped them feel comfortable.
Bailey F -
I STRONGLY recommend Dr. Bazzi. She is absolutely WONDERFUL. Very thorough, very nice, by far the best experience I've ever had with any doctor in my entire life. She specializes in anything that a woman would need. If anyone is interested I'd be happy to message you info on her because I'll never switch again. She's amazing!!!
Kyri B -
Dr Bazzi is amazing!! I honestly will never be able to thank her enough for saving my life. I will recommend her to every woman. Cannot say enough good things!
Bayli L




